
The Neuroscience of Meditation
November 14, 2020
The Microbiota-Gut-Brain Axis: Why Our Tummy Is Important for Our Mind
November 22, 2020COVID-19 Update: Part VI

In addition to emerging treatments and medications, which are reducing the mortality and possible long-term health consequences of COVID-19 and which I wrote about in the COVID-19 Knowledge Update #5, there are multiple social and logistical strategies we can, and should, employ in order to reduce the burden of COVID-19 and the need for prolonged lockdowns of the economy. Regarding economic lockdowns, the media’s portrayal of consensus among researchers is dishonest at best. I encourage readers to visit The Great Barrington Declaration and view the list of epidemiologists, virologists, and infectious disease experts (among many other experts) from some of the world’s most prestigious institutions that have initiated this declaration. Of note, some of them who previously signed advocating for the lockdowns in March, before we had the full data on the deadliness of the virus, are now retracting their positions and opposing the measures. They are not stating that the lockdowns do not work to curb the spread; they are stating that the lockdowns will cause more harm than good, from a public health and utilitarian perspective. The declaration is now signed by close to 12,000 medical and public health scientists and close to 34,000 medical practitioners, demonstrating that there is no consensus on the best approach.
Lifestyle
As I previously wrote about in COVID-19 Knowledge Update 3, there is an intimate relationship between sleep quality and immune function. There is good news, and bad news, regarding observations of our sleep patterns since the COVID-19 pandemic began. Potentially due to the large number of people working from home, total sleep length has increased by about 13 minutes,1 and “social jetlag,” which is a mismatch between an individual’s time spent on work and leisure in comparison to their internal biological clock, has declined.2 Dreaming has even increased, which could be considered beneficial at a first glance; however, upon deeper examination, the increased dreaming could indicate higher levels of stress and anxiousness.3 Despite increased sleep, decreased social jetlag, and increased dreaming, sleep quality appears to be down.2
It seems that one of the takeaways from the lockdowns, and shift to working from home, could have resulted in improved health by improving our sleep. Instead, the mounting stress (and perhaps decrease in physical activity) has evaporated this potential benefit. In addition to reduced physical activity, factors impairing sleep quality likely include increased alcohol consumption by as much as 54%4 and increased attention to the news media.5 Our health authorities should be relentlessly getting out the message that sleep quality is critical, especially during the pandemic, and encouraging behaviors that result in improved sleep quality.
In British Columbia, Canada, our always thoughtful and adroit government deemed liquor stores essential, while simultaneously fencing off parks. I know this was the case in many other areas, as well. It seems counterintuitive for any health authority to deem liquor stores, which became packed in frenzied panic buying, essential, yet to also deem the risk of walking through nature to be “too great of a risk.” High consumption of alcohol is well established to have adverse effects on the immune system.6 Who is responsible to ask the government these questions? The media.
The media has failed us during this pandemic in two ways. I’m going to stick with the mainstream left-leaning media in this regard, or rather, the side that believes the pandemic exists. They haven’t asked health authorities the hard questions or brought up controversy in pandemic response decisions from health authorities. Instead, they have used their platforms to parrot what we were told, and to denounce critical voices. I understand why this was done, as the voices claiming the pandemic does not exist are loud and potentially devastatingly harmful. However, by refusing to acknowledge shortcomings in public health decisions from our top doctors, the media is fanning the flames.
You may be wondering, “How does this play into the ‘lifestyle’?” If the media is simply sowing doom and gloom while not contributing to intellectual integrity, the net result is simply a constant barrage of chronic stress and anxiety — something about ¾ of those polled by ATTitude magazine state they are experiencing during the pandemic. This stress and anxiety are likely a causative factor in the trend of worsening sleep quality, which is well established to affect our immune system. If our health authorities were honest and pragmatic, they would be discouraging the population from watching the news during this pandemic, or at least until the news media changes their narratives and stops inciting fear, beyond the necessary concern and seriousness that the virus itself deserves, to boost ratings.
When the pandemic began, for most people, there was a sense of panic and lack of time. It was here, our health condition is our health condition, and there is not much we could do to change it. Now, 8 months later, we’ve learned a few things:
- It is likely that we will be infected with COVID-19 multiple times over our lives.
- The pandemic isn’t ending anytime soon. It may be another year before a vaccine has been administered to enough people to slow transmission.
- There is ample time left in the pandemic to either improve our metabolic health or let it fall apart.
It’s time for the various health authorities to aggressively advocate increased activity and exercise. Metabolic-related disorders are the most significant comorbidities for serious disease or death with COVID-19. Extended lockdowns and shutdowns of gyms, recreational sports, etc., will seriously impact many people’s health and fitness. These shutdowns are an important reason why activity decreased during lockdowns. Long-term consequences aside, the short-term consequences of COVID-19 are too serious to ignore. We need to be encouraging increased activity and exercise like never before. If you are reading this and your metabolic health is not ideal, it is not too late to take action. Start going for long walks. Start a light exercise program. Do anything you can to improve your metabolic health now, since when you will contract Covid-19, it will be too late to address and remedy. You’ll gain the added benefit of being healthier, happier, and reducing your risk for many diseases. Importantly, the metabolic factors are not the only potential benefit of exercise in relation to COVID-19 susceptibility. One study suggests that irisin, known as “the exercise hormone,” is able to modulate genes related to viral infection with COVID-19 for beneficial outcomes.7
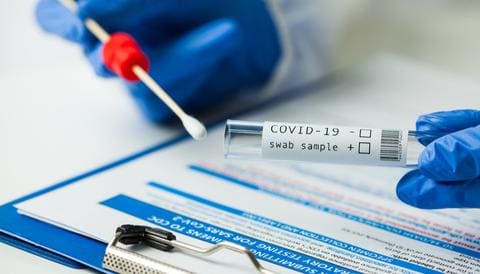
Testing Strategies
As we consider the successful coronavirus response in countries such as Taiwan, many North Americans assume that a strategy of mass testing and contact tracing to greatly impede the viral spread is no longer viable. However, this simply isn’t the case. China recently demonstrated the ability to test all 9 million citizens in Qingdao over 5 days, following just a dozen of positive tests. Widespread testing, unlike anything any politician has proposed, is our way out of this. It is also much cheaper than the alternative solutions. Let’s take a look at the two currently used methods, and some new methods available that could provide dramatic improvements.
PCR vs. Antigen Testing
To date, the gold standard for lab testing of the novel coronavirus has been PCR testing at approved laboratories, while the “rapid” tests have relied on antigen testing. PCR testing detects RNA of the virus, whereas antigen testing detects various molecules known to elicit an immune response.
PCR testing is more accurate than antigen testing; however, results can take days or even weeks due to a significant backlog at labs. Additionally, PCR tests may simultaneously be not sensitive enough for those who are asymptomatic, presymptomatic, or with mild symptoms, and also be “too sensitive,” detecting small amounts of the virus that pose no risk of infection for long after patients have recovered and cease to be contagious. This is likely due to the wide range of methods employed to conduct the test, with no one approved protocol.8 From STAT News:
“There was a lot of angst a few months ago about some people who had seemingly recovered from Covid-19 infections continuing to test positive for the virus for weeks. Were they infectious? Should recommendations be changed for how long infected people should be isolated?
It turns out it is an issue of testing. Most testing is conducted using a platform called PCR — polymerase chain reaction — that looks for tiny fragments of the SARS-CoV-2 virus. But the test can’t tell if those sections of genetic code are part of actual viruses that can infect someone else or fragments of viruses that are absolutely no threat.
It’s clear now that people who had mild or uncomplicated infections shed active viruses for somewhere up to 10 days after their symptoms started. (“Severely ill or immunocompromised patients do shed infectious virus for longer,” said Malik Peiris, a coronavirus expert at Hong Kong University.)
The weeks and weeks of positive tests — like those that prevented this woman in Quebec from cuddling her infant son for 55 days — don’t tell us that these people are still a risk to others. “In fact, we know that they are not infectious for that long,” said Maria Van Kerkhove, the World Health Organization’s leading coronavirus expert.”
This means that there is potentially a large percentage of people who are testing positive via PCR and do not need to quarantine, and were, in fact, positive and contagious before they receive results (even long before). There is also a large percentage of people gaining false negative tests.9 Conversely, antigen tests may be even less sensitive than the lowest sensitivity PCR tests with a reported false-negative rate as high as 50%! This means that someone may test negative for many days, while potentially contagious, before finally testing positive. Regarding the methods leading to highly sensitive PCR tests, the challenge is two-fold: decreasing time for delivery of results and determining detection limits for when an individual is contagious or recovered.
Highly-Sensitive and Fast Testing
Some new technologies are emerging, such as a portable machine that matches PCR lab accuracy and delivers results in 90 minutes. Another technology using CRISPR gene-editing technology that could be deployed to hospitals, office buildings, and schools is highly accurate, can determine precise levels of the virus, and can give results within 5 minutes This testing technology could be employed in large office buildings, hospitals, etc., as well as for the workforce, and using different test start times with a “wave” system could reduce backlogs in result delivery times. This would allow more businesses and workplaces to reopen, with less risk.
Yet another new testing technology currently being developed relies on a cheap sensor that eventually could be used within homes. The sensor can rapidly detect the coronavirus in less than 10 minutes, including in asymptomatic patients, while also providing useful data, such as antibody concentrations and inflammatory responses, to determine whether an individual is contagious and how serious their infection is. The sensor can also utilize multiple bodily fluids for testing, such as saliva, blood, or even sweat.
Yet another new cheap, portable technology matches PCR tests in accuracy and delivers results within 30 minutes, which can be sent directly to smartphones. While seemingly behind some other strategies, and only able to scale to a few hundred thousand tests in short order, utilizing multiple different testing methods simultaneously will no doubt be needed to ramp up nationwide testing programs.
Combining mass testing with contact tracing is an effective strategy, which could be made more effective if those who have come in contact with an infected individual could determine whether they are also infected before viral amounts are significant enough to trigger positive results in standard testing. New technology has been shown to be able to do just that, demonstrating improvements in sensitivity and the ability to detect far smaller viral loads.
Cheap Paper Tests
There is no question that the government bailouts will cause untold financial nightmares, which will, in turn, create health catastrophes in the coming years. Currently, various governments (including the USA and Canada) are incurring unfathomable debt, while only providing the bare minimum (or less) that citizens need to survive, with many individuals forced to stop working due to restrictions and lockdowns. As long as the pandemic continues, this debt will continue to rise. Further, large proportions of the bailout funding are being given to large corporations, further driving a class divide.
In the fall, the USA announced the purchase of 100 million tests, which sounds like a lot, but is far too little, and far too late. Rather than burning money while decreasing the quality of life, our governments could stimulate the economy and workforce by investing in scaling up new, rapid paper tests that could be used on all “active” citizens daily. This would create jobs and business ventures and allow for the complete reopening of society, at a fraction of the cost of the bailouts.
As reported by Harvard News, a Harvard epidemiologist argues for daily testing of all citizens with a cheap, although not perfectly accurate, paper test, which costs around $1. To provide some context, if 300 million Americans, or roughly 90% of the U.S. population, were tested daily, the cost per test would amount to $9 billion per month. After 1 year of testing, this amounts to half of the sum that has already been given in bailouts, not considering the additional bailouts on the way. Of course, there would be logistical expenses in distribution, app development, etc. Therefore, this cost could reasonably be doubled over the year. Of course, this “cost” would come with the benefit of reopening society, the incoming taxes from reopening, and additional jobs created.
Even at the estimated $6.85 per test that a similarly cheap, Indian-developed paper test costs, the benefits in mass testing far outweigh the costs, when considering bailouts and societal shutdowns. These tests could be scanned to an app, which gives individuals a “daily passport” to go about society, with checks for compliance at buildings, events, etc., which could be no different than ID checks. Falsification of test results may be an issue; however, commensurate fines and/or punishments could dissuade this practice.
The various federal governments could develop a system of cost; gainfully employed salaried taxpayers, students, and individuals actively seeking employment would be shipped the tests at no cost, while those who are not employed, seeking employment, or attending school would incur a small cost to purchase the tests.
As cheap paper tests could be easily used in daily life, the more accurate portable tests could be deployed to high-risk locations, such as nursing homes, with every individual being tested daily. This would mitigate the chances of asymptomatic staff members bringing the virus with them into a nursing home, where it could spread like wildfire among the high-risk inhabitants. If staffing becomes an issue, the military could be employed to assist in helping care homes conduct the testing. Additionally, family members wishing to visit could incur costs of the highly sensitive test, if resources are limited.
Additionally, the high-sensitivity portable tests could be purchased by those returning from international travel, to get tested at customs on arrival as an option over mandatory quarantines. The results would be electronically transmitted to them likely before they make it home. This would stimulate the airline industry, as well as international business. These tests with higher sensitivity could also be utilized for anyone identified through contact tracing to have come in close proximity to an individual that tested positive.
By utilizing a mass testing program, the virus could be contained within a matter of months, while society continues to operate as normal. This would create the necessary stopgap, while we wait for vaccine rollouts (in which compliance is likely to be low) as well as for more effective treatment options.
Immunity Passports
We still don’t know how long immunity lasts following the COVID-19 infection. Certainly, antibodies begin diminishing within a few months, but the T-cell response seems to last at least 6 months after infection. Considering there have only been a handful of examples of reinfection to date, a 180-day immunity passport could be instituted. This means that anyone who has tested positive previously could be omitted from the daily testing requirements, as well as from returning requirements after international travel, for up to 180 days following their positive test.
We could also develop a formula for scaling antibody testing and granting individuals a 90-day immunity passport based on their antibody levels. There are new antibody tests that are cheap and scalable, with new dried blood sampling tests also serving as an alternative and cheap option for antibody testing. This would immediately allow millions of individuals with test results on record, and perhaps tens of millions of individuals in the USA who subsequently take an antibody test to gain a temporary “immunity passport”, reducing the daily needs of the mass-scale paper test rollouts. This will also diversify the transfer of wealth and “winners” in the technological race in the fight with COVID-19.
We can reopen society safely. It will just take a concerted effort from our governments to develop plans of action that allow this to happen. By rolling out mass-scale daily testing, we will not only be able to reopen businesses and workplaces, but we will also be able to quickly snuff out community spread.
Next week, I will touch upon another strategy to reduce COVID-19 spread that has been contentious (to the public): The use of face masks. Are they dangerous? Are they effective? Should we be wearing them?
1. https://www.cell.com/current-biology/fulltext/S0960-9822(20)30837-X?_returnURL=https%3A%2F%2Flinkinghub.elsevier.com%2Fretrieve%2Fpii%2FS096098222030837X%3Fshowall%3Dtrue
2. https://www.scientificamerican.com/article/the-covid-19-pandemic-is-changing-our-dreams/
3. https://jamanetwork.com/journals/jamanetworkopen/fullarticle/2770975
4. https://www.forbes.com/sites/bradadgate/2020/08/21/nielsen-how-the-pandemic-changed-at-home-media-consumption/?sh=30b1ed2e5a28
5. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4590612/
6. https://europepmc.org/article/med/32593740





























1 Comments
I know your comment is benign however, Immunity passports will easily morph into vaccination passports and all the dystopia that comes with that. Tread lightly with that type of advice. Best Regards.