NREM and REM Sleep 101
September 6, 2022
Part 2 The Impact of Advanced Glycation End Products on Collagen
December 11, 2022Part 1 How Ultraviolet Radiation Damages the Skin and Causes Photoaging

The skin is the largest organ that serves as our primary protective barrier which interfaces with the external environment. It is constitutively exposed to various stimuli impacting its morphology and function, especially ultraviolet radiation (UVR). It has been reported that about 80% of skin aging can be attributed to UVR. Therefore, one of the best defenses against skin aging is diligent photoprotection.
Anatomy Of The Skin
The skin can be stratified into three major structural layers: the epidermis, the dermis and the hypodermis. Each of the cells within the skin have different proliferative capacities.
The epidermis is the outermost layer of the skin comprised of 5 layers:
- the stratum basale (the deepest portion of the epidermis)
- stratum spinosum
- stratum granulosum
- stratum lucidum
- stratum corneum (the top layer of the epidermis)
Cells that the comprise the epidermis are:
- Keratinocytes
- Melanocytes
- Langerhans’ cells
- Merkel’s cell
The dermis consists of two layers of connective tissue: the papillary and reticular layers, which merge together. The papillary layer is the upper part of the dermis composed of connective tissue. The reticular layer is the deeper portion that is less cellular and consists of dense connective tissue such as collagen.
The hypodermis, also referred to as the subcutaneous fascia, is the deepest layer of skin and contains adipose lobules along with hair follicles, sensory neurons, and blood vessels.
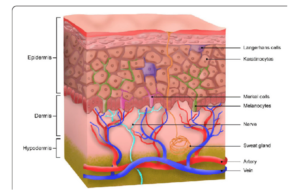
Photo credit: Yang et al., 2021
One of the most conspicuous ways that aging manifests itself is through the appearance of our skin. Skin aging is characterized by a cumulative loss of functionality and regenerative potential. It is a multi-factorial process that affects nearly every aspect of its biology and function. The skin is the most visible organ, where all changes, including aging, are very noticeable. The aging process of skin can be described as intrinsic (chronological) and extrinsic (elements in the environment). Unlike other organs of the human body, skin is not only impacted by intrinsic aging factors, but is also affected by extrinsic environmental factors. UVR imposes one of the most significant causes of extrinsic aging. This is known as photoaging, which is characterized by morphological changes including loss of elasticity, wrinkles, volume loss and redistribution of facial fat, and changes to the underlying structures of the skin. Photoaging is also characterized by histological changes such as dryness and alterations to the extracellular matrix, including disrupted collagen in the dermis.
Furthermore, Skin aging is associated with a compromised protective role; namely impaired wound healing and barrier function, increased inflammation, disrupted water and thermal homeostasis, and increased susceptibility to various skin disorders.
The Different Types of Ultraviolet Radiation
UVR can be broken down into various subtypes, each having a different deleterious impact on the skin.
- The longer waveband UVA (320-400 nm)
- UVA1 (340-400 nm)
- UVA2 (320-340 nm)
- The shorter waveband UVB (280-320 nm)
- UVC (100-280 nm)
- Blue-light/visible light (400-440 nm)
- Infrared (760-1200 nm)
UVC is absorbed in the stratosphere, and therefore, only UVA and UVB reach the surface of the earth (∼95% UVA, ∼5% UVB). Owing to its shorter wavelength, UVB rays are mostly absorbed by the stratum corneum in the epidermis (outermost layer of the skin) and are responsible for sunburns. UVB radiation is primarily a DNA-damaging agent because it is directly absorbed by DNA and causes the formation of cyclobutane pyrimidine dimers (CPDs) and 6-4 pyrimidine pyrimidone dimers (6-4PP).
Conversely, UVA rays. which are the most predominant, can penetrate into the deeper dermal layers of the skin and cause profound damage to DNA and other biomolecules. UVA has the strongest ability to generate reactive oxygen species (ROS) and lipid peroxidases, therefore causing destruction to collagen and elastin in the dermis. The major visible damaging effects of UVA radiation are cumulative and appear after years of exposure. UVA is principally responsible for photoaging.
Some evidence suggests that visible light and shorter waves of infrared (IR) light may also play a role in photoaging. Several studies have shown that Exposure to IR resulted in the typical clinical signs of photoaging.
How Ultraviolet Radiation Causes Damage To Skin
UVR exposure can induce tremendous insult to the skin in many ways.
Changes to Facial Fat
The morphology, distribution, and volume of subcutaneous facial fat is one of the hallmarks of a youthful phenotype. The structure and volume of the facial subcutaneous white adipose tissue undergo significant changes during aging, and this is accelerated by UVR. The changes in facial fat are depot specific and connected to a perturbed collagen network. One of the mechanisms by which UVR does this may be by decreasing expression of the adipokines leptin and adiponectin in the subcutaneous fat. A study by Ju Kim et al showed that UVR-induced silencing of adiponectin and leptin led to an upregulation of MMP-1 and decrease in type 1 procollagen expression. Treatment with adiponectin and leptin reversed these effects. UVR can also affect facial fat through inflammation. Photoinduced aging of facial fat also manifests as reduction of thickness, change of the intercellular matrix, quantitative and qualitative differences in preadipocytes.
Induction of Reactive Oxygen Species
UV-mediated ROS production is upstream of many of the mechanisms that lead to photoaging. UVR causes generation of reactive oxygen species (ROS) and DNA damage, resulting in cellular senescence, mitochondrial dysfunction, and a cascade of damage in the skin cells. Excess ROS drives global aging of the skin. It destroys cellular macromolecules such as proteins, lipids, as well as both nuclear and mitochondrial DNA. Excess ROS production by UVR can inundate the endogenous antioxidant capacity of the skin. This warrants the judicious use of exogenous antioxidants and other compounds as photoprotectants to mitigate UV-mediated ROS production. UVA is known to be the oxidizing component of the sun, and its destruction to biomolecules occurs indirectly through the generation of ROS via its interaction with a variety of chromophores. It has been demonstrated that the proteome is one of the major targets of damage by UVA-induced ROS.
Upregulation of Matrix Metalloproteinases
UVR increases the expression of matrix metalloproteinases (MMPs) in human skin. MMPs are enzymes that are responsible for degrading the extracellular matrix (ECM) proteins such as collagen, fibronectin, elastin, and proteoglycans. Dermal fibroblasts are the most abundant cell type in the dermis and are responsible for organizing the extracellular matrix. MMPs also play a pivotal role in photocarcinogenesis by influencing various processes related to tumor progression.
Damage to Mitochondrial DNA
UVR causes damage to both nuclear DNA and mitochondrial DNA (mtDNA), the latter being more vulnerable to destruction. The mitochondria plays a crucial role in skin aging. Berneberg and colleagues reported a 10-fold higher rate of a mtDNA deletion in photo-aged skin compared to sun-protected skin cells. In a subsequent study they published, repeated exposure of the skin to UVA increased the frequency of mtDNA aberrations in the dermis by 40% compared to unexposed skin. These UV-induced aberrations can persist over many years and continue to increase even in the absence of further UVR exposure. Repeated exposure to UVA radiation has been shown to result in mtDNA aberrations in skin cells, which manifests as mitochondrial dysfunction, increased activity of collagen-degrading enzymes (MMPs), and oxidative stress, which further instigates a vicious cycle of mitochondrial damage. UVR exposure promotes inhibition of procollagen synthesis and expedited collagen breakdown by UV-induced matrix metalloproteinases (MMPs) secreted from epidermal keratinocytes and dermal fibroblasts.
Cellular Senescence
Senescent cells in the skin can have detrimental effects through different mechanisms. UV exposure causes damage that ultimately leads to cellular senescence.UV-induced ROS can cause phosphorylation of kinases, resulting in the activation of MAPKs and subsequent downstream effectors. The activation of these kinases, in turn, upregulates transcription factors that increase the expression of MMPs, which are known senescence-associated secretory phenotype (SASP) factors. UV-induced senescent cells can alter the extracellular matrix as well as the physiology of the nearby cells, inciting photodamage and increased risk of skin cancer. The inflammatory cytokines IL-1α, IL-1β, ΙL-6, and TNF-α are highly secreted by senescent cells and have been reported to drive skin cancer by inducing the expression of angiogenic and invasion factors such as VEGF and MMP-1 through NF-κB signaling.
Summary
Our skin is our primary barrier against the environment that is regularly exposed to UVR and pollutants. Acute exposure to UVR causes sunburn, DNA damage, and immunosuppression. Chronic exposure to UVR, particularly UVA radiation, leads to the cumulative damage of premature photoaging. This results in decreased skin elasticity, wrinkles, hyperpigmentation, skin sagging, skin roughening, dryness, disrupted skin barrier, loss of facial volume, and many changes to the morphology of the skin.
UVR promotes photoaging and photocarcinogenesis through a variety of mechanisms that interplay with each other. UV-induced ROS triggers the cascade reaction of genes that promote inflammation, immunosuppression, mitochondrial dysfunction, and cellular senescence. Notably, it promotes the upregulation of matrix metalloproteinases which degrade and disrupt the integrity of proteins such as collagen and elastin. Collagen is the primary structural protein that gives resilience to the skin’s integrity. UVR promotes the breakdown of collagen and inhibits its synthesis. UVR also promotes the upregulation of pro-inflammatory cytokines, thereby inciting a cascade of cellular destruction in the skin cells.
Stay tuned for part 2 of this series to learn more about other major drivers of skin aging and ways to combat them.